We go to the doctor hoping to alleviate symptoms, understand a diagnosis, or receive treatment. However, something happens in that encounter that isn’t mentioned in medication leaflets: a human relationship is established. This relationship, known in health sciences as the Doctor-Patient Relationship (DPR). It is much more than a simple exchange of information between two people.
It is a bond that, when it functions well, improves clinical outcomes, reduces suffering, and humanizes care. When it fails, it can lead to errors, treatment abandonment, iatrogenic effects, and even lawsuits. Today, I invite you to explore what the DPR is, how it has evolved, what types exist. What both parties seek, and how we can strengthen this alliance that remains the very heart of Medicine.
Concept and History of the Doctor-Patient Relationship
The DPR is defined as the ethical, clinical, and communicative encounter between a healthcare professional (the doctor) and a person seeking help (the patient). It involves a convergence of technical knowledge, emotions, cultural values, and mutual expectations.
Historically, this relationship has gone through different stages. In antiquity, with Hippocrates, a paternalistic model predominated: the doctor knew what was best, and the patient trusted and obeyed. The Hippocratic Oath already established the obligation to do no harm and to act in the patient’s best interest.
During the Middle Ages and the Renaissance, patient-physician relationships remained based on trust, often tinged with religiosity. It was in the 20th century that three revolutions emerged: the technological (X-rays, antibiotics, laboratories), the legal (patient rights, informed consent), and the social (greater demands for transparency).
In 1992, bioethicists Emanuel and Emanuel systematized four models of patient-physician relationships that we still use to understand this evolution. Today, a biopsychosocial model is advocated, integrating the biological, psychological, and social aspects, along with shared decision-making.
Contexts in which this relationship occurs
The patient-patient relationship (PMR) doesn’t only happen in the doctor’s office; it manifests in multiple settings. Below, I discuss the most common ones.
Primary care: the family doctor or general practitioner, with continuity of care over time.
-
Hospitalization: in wards, emergency rooms, or operating rooms, with interdisciplinary teams.
-
Outpatient specialties: cardiology, endocrinology, oncology, psychiatry, etc.
-
Telemedicine: telephone or video consultations (a growing context post-Covid-19 pandemic).
-
Palliative and end-of-life care: where communication is central to comfort and dignity.
-
Preventive medicine: in vaccination campaigns, checkups, and lifestyle advice.
Each context imposes its own rules regarding time, privacy, and technological support.
Types of Doctor-Patient Relationships (Classic Models)
According to Emanuel and Emanuel, the four main models are as follows:
- Paternalistic: The doctor decides what is best, and the patient obeys without question (parent-child).
- Informative: The doctor provides objective data, and the patient chooses for themselves (salesperson-customer).
- Interpretive: The doctor helps clarify values and preferences.While the patient decides according to their own values (counselor-client).
- Deliberative: The doctor recommends, argues, and persuades alongside the patient. Alsowho actively participates and deliberates (partner-partner).
In practice, the same doctor may use different models depending on the situation. For example, a more paternalistic approach in a cardiac arrest, a more deliberative approach when deciding on cancer treatments. In other words, it depends on the case.
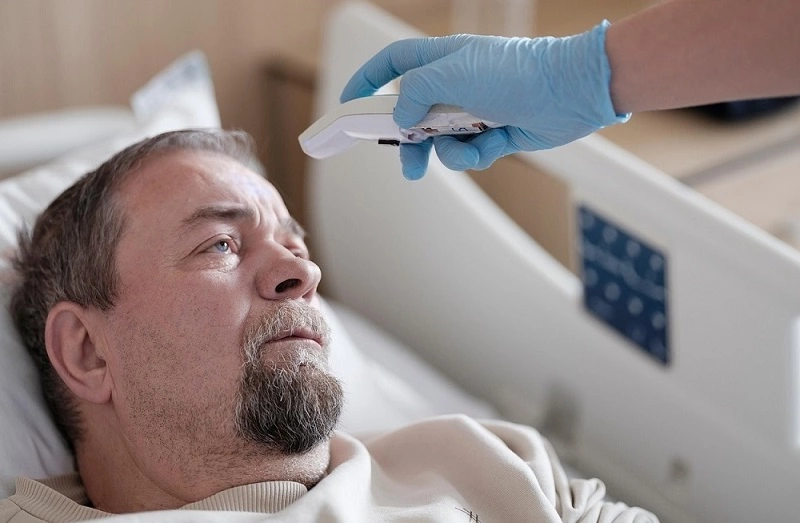
Patient and Doctor Goals
Although both share the desire to heal or alleviate suffering, their perspectives may differ. Let’s take a look.
Patient Goals: To be listened to without rushing, to receive clear and understandable information. Also to be treated with respect and dignity, to participate in decisions about their body, to obtain symptom relief or a cure, and to maintain trust in the professional.
Doctor Goals: To establish an accurate diagnosis, to offer the best available treatment (based on evidence). To avoid harm (principle of non-maleficence), to respect the patient’s autonomy, to optimize time and resources, and to facilitate adherence to treatment.
When these goals are aligned, satisfaction and outcomes improve significantly.

The doctor-patient relationship is not a luxury or a matter of good manners: it is an active component of therapy. Scientific evidence shows that a good doctor-patient relationship improves adherence, reduces clinical errors, decreases physician burnout, protects patients from iatrogenic harm, and leads to better outcomes. Despite increasing technology, limited time, and bureaucracy, it is the human connection that sustains the medical act. Healthcare professionals must pay attention to listening, empathy, and the therapeutic alliance as essential competencies, not as mere embellishments.
- The Doctor-Patient Relationship: A Highly Meaningful and Sensitive Interpersonal Relationship - 4 de May de 2026
- Beyond the White Lie, Fiction Takes Over Identity - 27 de April de 2026
- The Son: When love can’t conquer all and looking the other way is useless - 22 de April de 2026

